
- Press Releases
- Industry Updates
- SIMTech Manufacturing Matters
- Manufacturing Matters
- SIMTech 30th Anniversary
- Events
- ASPEN2022
- BCA Green Mark (Platinum) for Healthier Workplaces and Laboratories
Better Bone Implants with 3D Printing
Binder jetting of Mg-based and Ti-based materials – the future of orthopaedic implants processing
Demand for orthopaedic devices is thriving, primarily due to aging population where there is a higher occurrence of age-related conditions like osteoarthritis, leading to injuries requiring orthopaedic devices. Additive manufacturing (AM), also known as 3D printing, has been developing very rapidly into a game-changing technology for biomedical applications as it allows for unprecedented design freedom for fabrication of patient-specific implants.
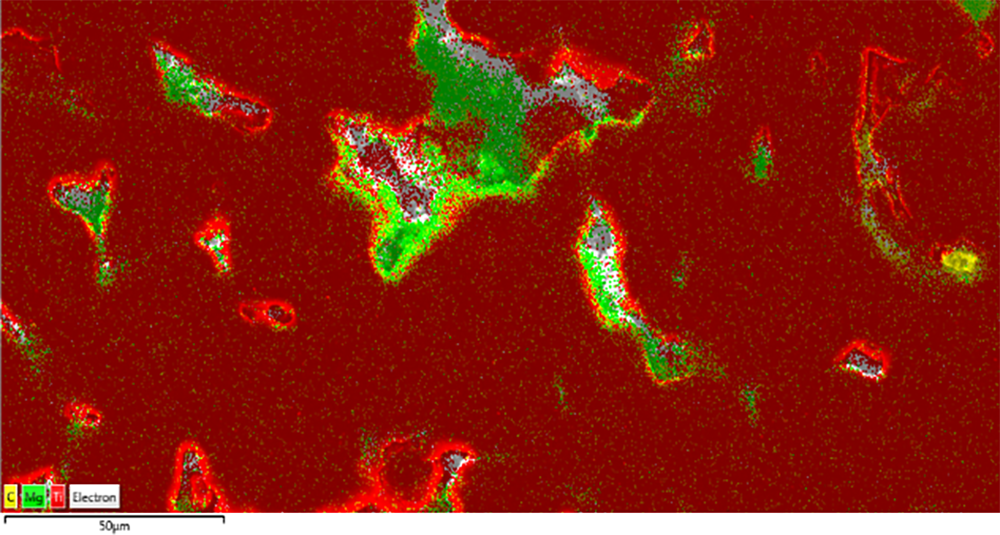
Magnesium (Mg) is a biodegradable metal. When Mg is implanted, it degrades and is eliminated safely from the body over a period of time, as compared to permanent implant materials such as Titanium (Ti) and Cobalt-Chromium alloys. However, Mg’s inherent properties – such as high affinity to oxygen and low boiling temperature – make it one of the most challenging materials for AM processing. Currently, Mg material and processing is not offered by any AM’s original equipment manufacturer.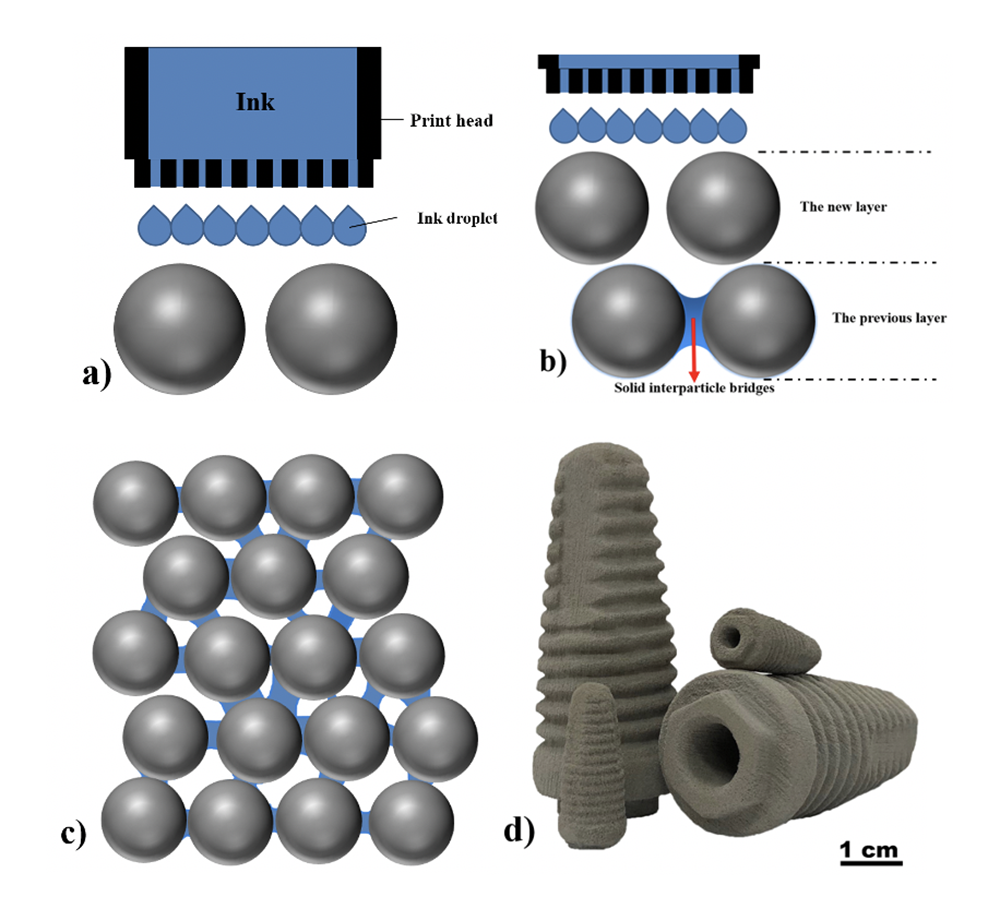
Fig. 1. The process flow for binder jetting of degradable Mg implants, a) depositing the ink into the overspread layer of powder, b) forming a solid inter-particle bridge in the previous layer of powder and deposing the ink into a designated area of the new layer of powder, c) repeating steps a and b to build the entire implant, and d) the macrograph of screws made of Mg powder.
In collaboration with NUS, SIMTech team has developed a unique binder jetting printing (BJP) process work flow (see Fig. 1) for AM of Mg, involving capillary-mediated binder-less BJP to form green Mg parts at near-ambient temperature and then transforming the green parts into functional components via sintering process. This enables the fabrication of interconnected open-porous structures of Mg-based alloys that have comparable mechanical properties and porous characteristics to those of human cortical bone types. However, Mg resorbable implants degrade spontaneously under aqueous medium and controlling its degradation rate is difficult due to the presence of high concentrations of chloride ions within the human body. The next stage of research and development will focus on the approaches to better control the degradation rate.
Among the permanent implants, Ti alloys have been widely employed for direct bone replacement due to their high specific strength and corrosion resistance within the human body environments. However, Ti materials exhibit high Young’s modulus (105GPa) leading to stress shielding effects, and insufficient osteointegration with the connecting bone during the early stages of implantation. These factors cause pre-mature failure of implants.
In another collaboration to improve the implants, SIMTech and NUS successfully developed a hybrid implant solution by combining the stronger BJP Ti interconnected open-porous structures matrix and subsequently filling the pores with low modulus and biodegradable Mg via capillary mediated infiltration. Over time, the Mg phase in the implant will improve osteointegration with the connecting bone and slowly degrades, leaving behind open pores within the Ti implant, favouring bone in-growth. The fabricated Ti + Mg composites exhibited superior compression properties with high ultimate compressive strength and low Young’s modulus properties, matching that of the human cortical bone.
In recognition of the scientific novelty and potential applications, these works have been published in the Materials Science and Engineering: C, Acta Materialia, Materials & Design, Additive Manufacturing and reported by professional media.
Current developments in BJP of Mg-based and Ti-based materials can help to accelerate the demonstration and adoption of 3D printed implants in the medical field.
For more information, please contact Dr Seet Hang Li, Section Manager, Metal & Ceramic Forming Group at seet_hang_li@SIMTech.a-star.edu.sg
A*STAR celebrates International Women's Day

From groundbreaking discoveries to cutting-edge research, our researchers are empowering the next generation of female science, technology, engineering and mathematics (STEM) leaders.
Get inspired by our #WomeninSTEM
.png?sfvrsn=843a4005_8)